Arthroscopic ACL Reconstruction
KNEE
Introduction to ACL Injuries
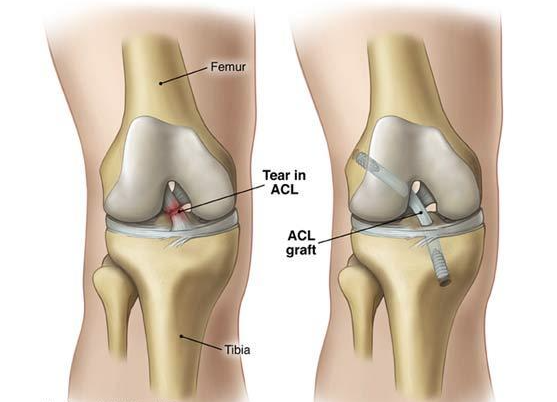
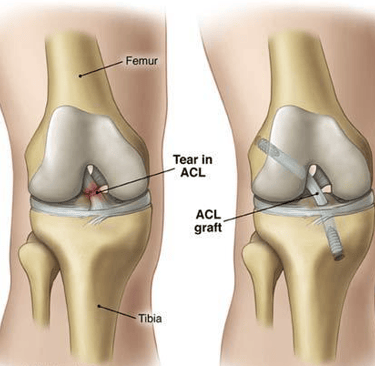
The anterior cruciate ligament (ACL) plays a critical role in maintaining the stability and functionality of the knee joint. Located in the center of the knee, this ligament connects the thigh bone (femur) to the shin bone (tibia), allowing for effective movement and support during various physical activities. The ACL is essential for activities that involve sudden changes in direction, jumping, and quick stops, which are common in many sports. Consequently, injuries to the ACL can significantly affect one’s mobility and overall quality of life.
ACL injuries often occur due to a combination of factors, including the mechanism of impact, anatomical predisposition, and physical conditioning. Common causes include sports-related incidents, such as twisting movements, landing awkwardly from jumps, or collisions with other players. Non-sport-related causes, such as accidents or falls, can also lead to ACL disruptions. Studies indicate that these injuries are particularly prevalent in sports such as football, basketball, and soccer, where rapid movements and agility are key components of performance.
The impact of an ACL injury extends beyond the immediate physical limitations; it can lead to long-term consequences, such as osteoarthritis, decreased range of motion, and an overall reduction in activity levels. This progressive decline can adversely affect an individual’s mental well-being and social life, leading to increased instances of depression or anxiety related to physical inactivity. The importance of understanding ACL injuries thus becomes apparent, as it underscores the need for timely diagnosis and appropriate treatment options, including potential surgical procedures like ACL reconstruction, to restore function and enhance the quality of life for affected individuals.
Indications for ACL Reconstruction
Anterior cruciate ligament (ACL) reconstruction is a surgical procedure indicated for patients who have sustained injuries to this crucial ligament in the knee. The decision to recommend ACL reconstruction is typically based on several factors, primarily the severity of the knee injury, the patient’s age, activity level, and the presence of associated knee injuries. Complete tears of the ACL, characterized by a total rupture of the ligament, tend to warrant surgical intervention due to the significant instability they cause in the knee joint. In contrast, partial tears may occasionally respond well to non-surgical treatments such as physical therapy and bracing.
The severity and nature of the ACL injury play a critical role in treatment decisions. Athletes or individuals with physically demanding lifestyles who experience complete tears are often advised to undergo knee reconstruction. This is due to the fact that instability can lead to further joint damage and complications if left untreated. Conversely, for recreational athletes or individuals with less physically demanding lifestyles, conservative management might be suggested, especially if the ACL injury is partial and accompanied by minimal instability.
Additionally, age is a significant consideration in the recommendation for surgery. Younger patients, particularly those engaged in sports, are generally more likely to undergo ACL reconstruction to restore the knee’s stability. Older patients may be given a different perspective, particularly if they have other comorbidities or less active lifestyles. The presence of other knee injuries, such as meniscal tears or articular cartilage damage, can also impact the decision, as addressing these issues during ACL reconstruction may improve overall outcomes. Each case is evaluated individually, with a thorough assessment ensuring that patients are informed of the best options for their specific situations.
Surgical Options for ACL Reconstruction
Anterior cruciate ligament (ACL) reconstruction is a critical procedure for individuals suffering from ACL injuries, with various surgical techniques available to address this prevalent issue. The two primary types of graft options are autografts and allografts. An autograft utilizes tissue taken from the patient’s own body, typically sourced from the patellar tendon, hamstring tendon, or quadriceps tendon. Conversely, an allograft employs tissue from a deceased donor, which is processed and sterilized for surgical use.
Each graft option presents unique advantages and disadvantages. Autografts generally offer improved integration with the patient’s body and reduced risk of disease transmission since the tissue originates from the patient themselves. However, harvesting autografts can lead to additional discomfort and potentially longer recovery times due to the dual surgical sites. In contrast, allografts minimize surgical morbidity, eliminate the need for harvesting, and can lead to shorter operation times and quicker initial recovery. Nevertheless, they carry a slightly higher risk of graft failure and may not integrate as effectively as autografts.
The surgical procedure timeline typically begins with a thorough preoperative assessment, which may include imaging studies and consultations to determine the most suitable graft option. Anesthesia is administered before the surgeon repairs the torn ligament using the selected graft. The procedure usually lasts between one to two hours, followed by a recovery phase in which the patient is monitored for any complications. Post-surgery, a structured rehabilitation program is essential, commencing with gentle exercises aimed at restoring motion and gradually increasing strength.
Ultimately, the choice of surgical technique must be tailored to the individual patient’s specific needs, lifestyle, and activity level. Engaging in open dialogue with the healthcare team is crucial to ensure an informed decision regarding the preferred surgical option for ACL reconstruction.
Post-Operative Rehabilitation Process
The post-operative rehabilitation process following ACL reconstruction is crucial for a successful recovery. It typically entails several stages, beginning with initial recovery and progressing through strengthening exercises, ultimately leading to a return-to-sport phase. Each step is designed to restore function, improve stability, and enhance the overall outcomes for the patient.
Initially, the focus is on managing inflammation and pain control, which can last for several days to a week post-surgery. During this phase, weight-bearing activities are often restricted, and patients are encouraged to perform gentle range-of-motion exercises. Physical therapy plays a vital role in guiding patients through this initial period, ensuring that the knee regains mobility without stressing the surgical site.
As patients advance to the strengthening phase, typically around six weeks post-operation, the rehabilitation program transitions to more targeted exercises aimed at rebuilding muscle strength and stability around the knee joint. These exercises may include closed-chain movements, resistance training, and balance activities. Physical therapists customize programs to suit individual recovery rates and conditions, emphasizing the importance of consistent practice to optimize results.
The return-to-sport phase is carefully monitored and typically begins around six to nine months post-surgery, depending on the individual's progress and specific sport requirements. Before resuming competitive activities, patients must meet defined criteria, including adequate strength, stability, and functional movement patterns. Regular assessments by the rehabilitation team help ensure that each patient meets these benchmarks safely.
Several factors can influence the success of rehabilitation, including age, pre-injury activity level, and adherence to the rehabilitation protocol. Consequently, it is essential that patients actively engage with their rehabilitation process, attend scheduled physical therapy sessions, and follow prescribed exercise regimens. By prioritizing a comprehensive rehabilitation strategy, patients can effectively enhance their recovery outcomes post-ACL reconstruction.
Patient Information and Expectations
Undergoing ACL reconstruction is a significant decision that involves careful consideration and preparation. It is essential for patients to be thoroughly informed about what to expect in the lead-up to, during, and following the surgical procedure. Prior to surgery, patients will usually undergo a comprehensive assessment, which may include imaging studies or consultations with healthcare professionals. These evaluations help ensure that the surgery is appropriate for the patient's specific condition.
Pre-operative preparations are crucial for a smooth surgical experience. Patients are often advised to abstain from certain medications, such as blood thinners, and to follow specific dietary instructions leading up to the procedure. It is also beneficial for patients to organize their home environment to facilitate a more comfortable recovery. Having ice packs, pain medication, and mobility aids ready can make a significant difference once they return home.
The hospital stay typically ranges from outpatient care to a few days, depending on individual circumstances. During the operation, anesthesia is administered, and the patient should feel little to no discomfort. Post-surgery, a personalized pain management strategy will be important. This may include medications such as opioids for intense pain initially, transitioning to over-the-counter options as prescribed by the surgical team. Ice applications and elevation of the leg can also be effective in reducing swelling and managing pain.
After ACL reconstruction, it is crucial for patients to be vigilant regarding signs of complications. This may include excessive swelling, increased pain, fever, or any unexpected changes in their condition. Adhering to follow-up appointments and maintaining open communication with the healthcare team will facilitate a more effective recovery. Setting realistic expectations for timelines and recovery milestones will help alleviate concerns and promote adherence to rehabilitation protocols.
Long-Term Outcomes and Risks
The long-term outcomes of anterior cruciate ligament (ACL) reconstruction are vital for patients considering this surgical intervention. Most studies suggest that approximately 80% to 90% of individuals return to their previous level of physical activity or sports within the first two years post-surgery. The success of ACL reconstruction is influenced by various factors, including the patient's age, activity level, and adherence to rehabilitation protocols. Athletes, particularly those in high-demand sports, often report satisfactory outcomes, yet this demographic may still experience a heightened risk of subsequent injuries.
In terms of knee function, many patients report significant improvement, with enhanced stability and diminished pain. However, it is crucial to recognize that not all patients achieve the same level of post-operative function. Some may experience lingering issues such as stiffness, swelling, or decreased range of motion, which could affect their long-term quality of life. Additionally, meta-analyses indicate that the rate of reinjury, particularly to the same knee, ranges from 5% to 15%, necessitating specific focus on injury prevention strategies during rehabilitation.
Despite the many successful outcomes associated with ACL reconstruction, the surgical procedure is not without risks. Potential complications include infection, blood clots, and adverse reactions to anesthesia. Furthermore, some studies suggest a possible link between ACL reconstruction and the eventual development of osteoarthritis (OA) in the affected knee. This has prompted ongoing discussions regarding the importance of post-surgical joint health and the need for regular monitoring even after rehabilitation is complete.
Overall, while ACL reconstruction can significantly improve patients' knee function and allow a return to sports, understanding the potential risks and realistic expectations for long-term outcomes is vital. A comprehensive approach to rehabilitation and continuous assessment of joint health are essential to optimize recovery and minimize future complications.
Conclusion and Final Thoughts
In summary, understanding ACL reconstruction is paramount for both patients and healthcare providers. The anterior cruciate ligament (ACL) serves a critical role in knee stability, and its injury can significantly impact an individual's daily activities and overall quality of life. Knowledge of the various indications for surgery, including the severity of the ligament tear and the patient's lifestyle demands, is essential when considering the appropriate management strategy.
Moreover, the rehabilitation process following ACL surgery is equally important for ensuring a successful recovery. Adhering to a structured rehabilitation regimen not only facilitates healing but also strengthens the knee to withstand future physical demands. Patients are encouraged to actively engage in their rehabilitation program and maintain open communication with their healthcare professionals. This dialogue is crucial for addressing concerns, adjusting recovery plans, and achieving optimal outcomes.
Healthcare professionals must also stay informed about the latest advancements in ACL reconstruction techniques and rehabilitation protocols. This knowledge allows them to provide the best possible care, tailored to the unique needs of each patient. By prioritizing ongoing education and collaboration, both patients and providers can foster an environment conducive to healing and resuming an active lifestyle.
Ultimately, understanding the complexities surrounding ACL reconstruction enhances both awareness and preparedness for those undergoing this procedure. It empowers patients to take charge of their recovery journey while fostering an atmosphere of trust and cooperation with their healthcare team. By embracing this holistic approach, individuals can significantly improve their chances of a successful rehabilitation and a return to their desired activities.
