Pelvi-Acetabular Fractures
Introduction to Pelvi-Acetabular Fractures
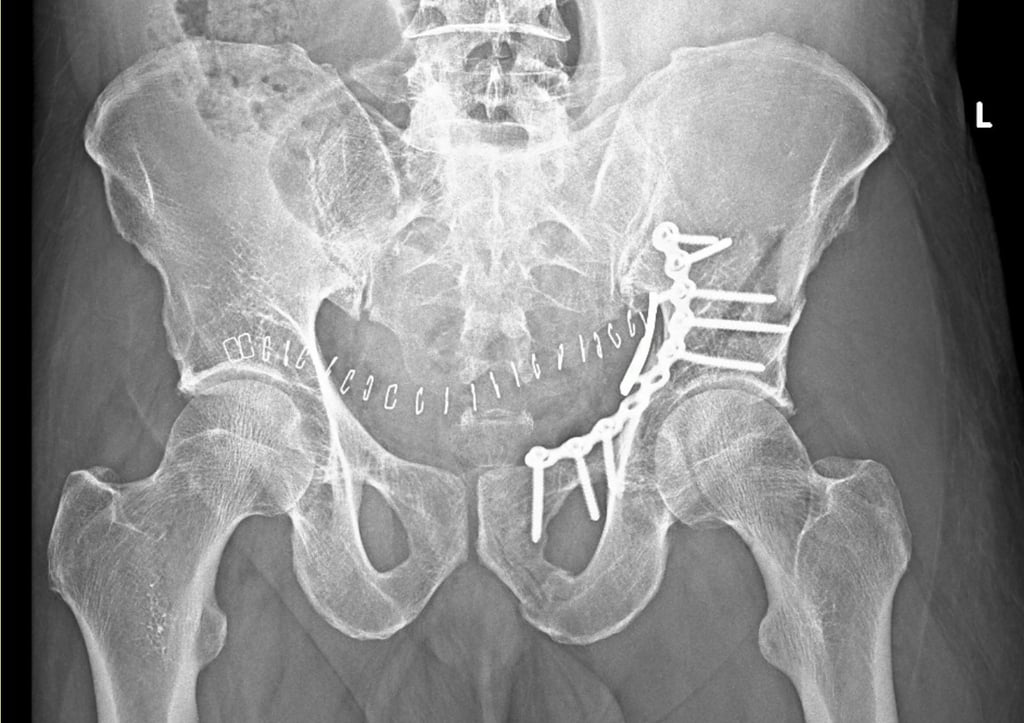
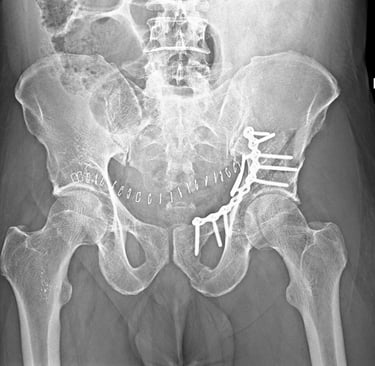
Pelvi-acetabular fractures represent a significant category of orthopedic injuries, characterized by fractures occurring in the pelvic ring and the acetabulum, which is the socket portion of the hip joint. These fractures typically arise as a consequence of high-energy trauma, such as vehicular accidents, falls from heights, or sports injuries. Given the anatomical complexity of the pelvis and the critical role it plays in weight-bearing and ambulation, understanding these fractures is essential for Orthopaedic surgeons.
Anatomically, the pelvis is a resilient structure composed of several bones, including the ilium, ischium, pubis, sacrum, and coccyx. The acetabulum, a cup-shaped structure located at the junction of the ilium, ischium, and pubis, serves to accommodate the femoral head, facilitating hip movement and providing stability. Because of this intricate configuration, any injury to the pelvis or acetabulum may lead to significant functional impairment and long-term consequences for affected individuals.
The mechanism of injury for pelvi-acetabular fractures varies, but the most frequent causes involve high-impact forces. Due to the nature of these injuries, they predominantly affect younger male populations, especially in active age groups, although they may also occur in elderly individuals through falls. The significance of pelvi-acetabular fractures extends beyond immediate injury; they can result in complications such as hemorrhage, nerve damage, and long-term disability if not promptly and effectively managed.
Furthermore, the proper diagnosis and treatment of pelvi-acetabular fractures are essential, as they can significantly affect patient outcomes. Given the traumas associated with these fractures, familiarity with their mechanisms, prevalence, and implications forms the foundation for effective trauma care and rehabilitation strategies. Understanding these fractures is crucial for optimizing treatment protocols and improving recovery trajectories for affected patients.
Incidence and Epidemiology of Pelvi-Acetabular Fractures
Pelvi-acetabular fractures represent a significant group of injuries with varying incidence rates across demographics and regions. Epidemiological studies have consistently shown that these fractures are more prevalent among older adults, particularly those over the age of 65. The increased incidence in this age group is primarily linked to factors such as diminished bone density, which is often exacerbated by osteoporosis. Gender disparities are also evident, with men experiencing these fractures at a higher rate than women, influenced by risk-taking behaviors and higher participation in contact sports.
Statistical data indicates that pelvi-acetabular fractures are frequently the result of high-energy trauma, such as vehicular accidents or falls from significant heights, which are more common in urban settings. As per recent studies, nearly 70% of these fractures occur due to traffic collisions, while falls account for about 25%. Additionally, sports-related injuries, particularly in active individuals aged 18 to 35, contribute to the incidence of these fractures.
Over the decades, the trend of pelvi-acetabular fractures has been evolving. In recent years, there has been an increase in fractures associated with low-energy falls, pointing towards an aging population at risk. Moreover, advancements in emergency care have also led to improved identification and diagnosis of these injuries, potentially contributing to higher reported incidence rates. It is essential to consider the influence of external factors, such as socioeconomic status and access to healthcare, as they can significantly affect the reported prevalence of these injuries.
In summary, understanding the epidemiological landscape of pelvi-acetabular fractures is crucial for developing targeted strategies in prevention and management, especially as demographic dynamics continue to shift. Awareness of the contributing factors, along with statistical insights, will aid in mitigating the risks associated with these potentially debilitating injuries.
Initial Emergency Care for Pelvi-Acetabular Fractures
When a pelvi-acetabular fracture is suspected, immediate and effective emergency care is critical to mitigate complications and enhance patient outcomes. The initial assessment begins with a thorough evaluation of the patient's overall condition, including vital signs, level of consciousness, and the presence of any life-threatening injuries. A focused examination should be conducted to identify the location of pain, assess movement, and detect any signs of neurovascular compromise.
Pain management plays a vital role in the emergency treatment of pelvi-acetabular fractures. Administering appropriate analgesics not only aids in patient comfort but also allows for more accurate evaluations and assessments. This can often require the involvement of trained professionals to determine safe, effective medication dosages while considering the patient's medical history and potential contraindications.
Following pain management, initial imaging, such as X-rays and, if necessary, CT scans should be performed to confirm the diagnosis and understand the extent of the fracture. These imaging studies will guide treatment plans and provide critical information for surgical teams. Trauma teams must prioritize these imaging studies to make appropriate decisions swiftly.
Stabilization of the patient is another crucial component of emergent care for pelvi-acetabular fractures. This step may include managing any associated internal or external bleeding, immobilization of the pelvis, and ensuring the surrounding structures are adequately supported. Trauma teams often employ traction methods or pelvic binders to reduce movement and further complications.
In emergency settings, timely triage is essential. Larger trauma centers usually have specialized trauma teams capable of assessing and managing fractures. These teams work collaboratively to ensure that the patient receives appropriate care that aligns with best practices in emergency medicine. Prompt identification of their needs and swift action can significantly reduce mortality and improve the chances of a successful recovery.
Surgical Treatment Options for Pelvi-Acetabular Fractures
Surgical intervention is a critical component in the management of pelvi-acetabular fractures, as these injuries often lead to significant morbidity and complications if not addressed appropriately. The primary surgical technique utilized is open reduction and internal fixation (ORIF), which aims to restore anatomical alignment and stabilize the fracture. ORIF is indicated for specific fracture patterns, such as those involving displacement of the acetabulum or significant instability of the pelvic ring. This approach allows for early mobilization and enhances the prospect of functional recovery.
Another surgical option involves percutaneous fixation, which has gained popularity due to its minimally invasive nature. This technique is particularly advantageous in patients with soft tissue concerns or comorbidities that complicate traditional surgical approaches. Percutaneous fixation may not offer the same fine control over fracture alignment as ORIF, but it reduces the risk of complications associated with extensive soft tissue dissection.
The choice of surgical method is largely influenced by the type and severity of the fracture, the patient’s overall health, and the presence of any concurrent injuries. A thorough assessment and imaging studies help guide orthopedic surgeons in determining the most appropriate strategy. Potential advantages of surgical treatment include pain relief, restoration of joint function, and decreased risk of post-traumatic arthritis. Nonetheless, challenges such as the risk of infection, nonunion, and other complications must be considered when planning surgical treatment.
Postoperative care is vital for successful recovery following surgical intervention for pelvi-acetabular fractures. Patients typically require a tailored rehabilitation program that addresses mobility, strength, and flexibility, along with regular follow-up to monitor the healing process. Overall, the surgical treatment of these complex fractures requires a multifaceted approach to ensure optimal outcomes for patients.
Rehabilitation After Pelvi-Acetabular Fractures
Rehabilitation following surgical intervention for pelvi-acetabular fractures is essential to restore function and mobility. The primary goals of this rehabilitation process are to reduce pain, enhance physical function, promote tissue healing, and facilitate a safe return to daily activities. A structured rehabilitation program is crucial for achieving these objectives and varies based on the severity of the fracture and the surgical techniques employed.
The rehabilitation timeline typically begins immediately post-surgery, focusing on gentle movement to prevent stiffness and promote blood circulation. Early mobilization is often introduced within the first few days post-operation, with patients gradually progressing to weight-bearing activities as tolerated, usually within weeks to a couple of months depending on individual recovery. Full rehabilitation can take several months, often assessing the patient's progress regularly to adjust the program accordingly.
A multidisciplinary approach is vital for optimizing recovery outcomes. This may include physiotherapists who design specific exercises aimed at improving mobility, strength, and posture, and occupational therapists who assist in adapting daily living activities to the patient’s current capabilities. These specialists work collaboratively to ensure that patients regain independence and confidence in their movements.
Strategies to improve mobility commonly involve a combination of strength training, flexibility exercises, and functional training that simulates daily activities. This not only aids physical recovery but also addresses mental well-being, which is often a neglected aspect of rehabilitation. Monitoring for complications, such as joint stiffness or pain, is an integral part of the rehabilitation process to adapt strategies as necessary.
Overall, a structured, multidisciplinary rehabilitation program tailored to the individual patient's needs is vital in promoting recovery and ensuring a successful return to pre-injury levels of activity.
Long-term Outcomes and Complications
The long-term outcomes for patients who have experienced pelvi-acetabular fractures are influenced by a multitude of factors, including the severity of the fracture, the effectiveness of the initial treatment, and the presence of any comorbid conditions. These fractures, which affect the pelvic ring and hip joint, can lead to complex recovery trajectories, potentially complicating rehabilitation efforts and impacting patients’ overall quality of life.
One of the most prevalent complications observed in individuals recovering from pelvi-acetabular fractures is post-traumatic arthritis. This condition arises when the cartilage in the hip joint is damaged during the injury, leading to inflammation and eventual degeneration of joint surfaces. Evidence suggests that the incidence of post-traumatic arthritis can be considerably high, even when fractures are treated surgically. Long-term follow-up studies indicate that patients may develop symptoms years after the initial injury, underscoring the importance of continuous monitoring and management of joint function.
Moreover, the healing process can be adversely affected by pre-existing comorbid conditions such as obesity, diabetes, and osteoporosis. These conditions can impair bone healing, prolonging recovery and increasing the likelihood of complications. Research underscores the need for a comprehensive evaluation of each patient’s health status before and after treatment to optimize rehabilitation outcomes. A proactive approach that integrates physical therapy, dietary modifications, and lifestyle changes may significantly enhance the recovery trajectory.
Recent studies have provided insights into patient quality of life following these injuries, revealing that many individuals struggle with persistent pain, reduced mobility, and difficulties in performing daily activities. Such findings highlight the necessity for a multidisciplinary approach to treatment, which can encompass surgical intervention, rehabilitative care, and psychological support. Continuous research into the long-term outcomes of pelvi-acetabular fractures remains critical in improving treatment protocols and enhancing the lives of affected individuals.
Conclusion and Future Directions
In conclusion, the management of pelvi-acetabular fractures encompasses a multifaceted approach that includes assessment of incidence rates, emergency care protocols, surgical interventions, and rehabilitation strategies. Throughout this blog post, we have addressed the critical importance of prompt diagnosis and treatment to mitigate complications associated with such fractures. Key points highlight that timely emergency care is essential for stabilizing patients and preventing further injuries, while surgical treatment remains a cornerstone in managing more complex cases.
Current research trends are revealing advancements in techniques and technologies aimed at improving surgical outcomes for pelvi-acetabular fractures. Emerging treatments, such as minimally invasive surgical methods and enhanced postoperative rehabilitation protocols, are likely to shape the future of patient care in this field. These innovations not only aim to expedite recovery but also to enhance overall functionality and quality of life post-injury. Studies examining long-term outcomes and rehabilitation effectiveness are instrumental in delineating best practices and informing treatment guidelines.
Looking ahead, several questions arise regarding future directions in the management of pelvi-acetabular fractures. How might the integration of telemedicine and remote monitoring improve patient follow-up and outcomes? What role will multidisciplinary teams play in optimizing care paths for affected individuals? The importance of continued education and awareness among healthcare professionals cannot be overstated, as it directly influences the quality of care provided to patients. It is essential for practitioners to stay abreast of emerging research and innovations, ensuring that they can efficiently manage pelvi-acetabular fractures. As we navigate the evolving landscape of orthopedic trauma care, fostering a commitment to knowledge advancement will be critical in providing optimal patient outcomes.
